How Pharmacy Benefit Managers Shape Prescription Coverage
Pharmacy Benefit Managers administer prescription drug benefits on behalf of insurers, employers, and public programs. Their decisions influence which medications are covered, what patients pay, and how prescriptions are dispensed.
Patients Rising believes lasting healthcare reform requires collaboration across the entire system. Our role is to bring forward the patient perspective and help ensure policies improve access, affordability, and outcomes for the people the healthcare system exists to serve.

What PBMs Do
Pharmacy Benefit Managers administer prescription drug benefits on behalf of health insurers, employers, and government programs. They negotiate prices with manufacturers, design formularies, and coordinate pharmacy networks.
Why PBMs Matter
Because PBMs help manage prescription coverage for more than 200 million Americans, their policies directly influence how patients access medications and what they pay at the pharmacy.
What’s Changing
New federal legislation has introduced reforms designed to increase transparency and curb controversial PBM practices, particularly in Medicare and Medicaid programs.
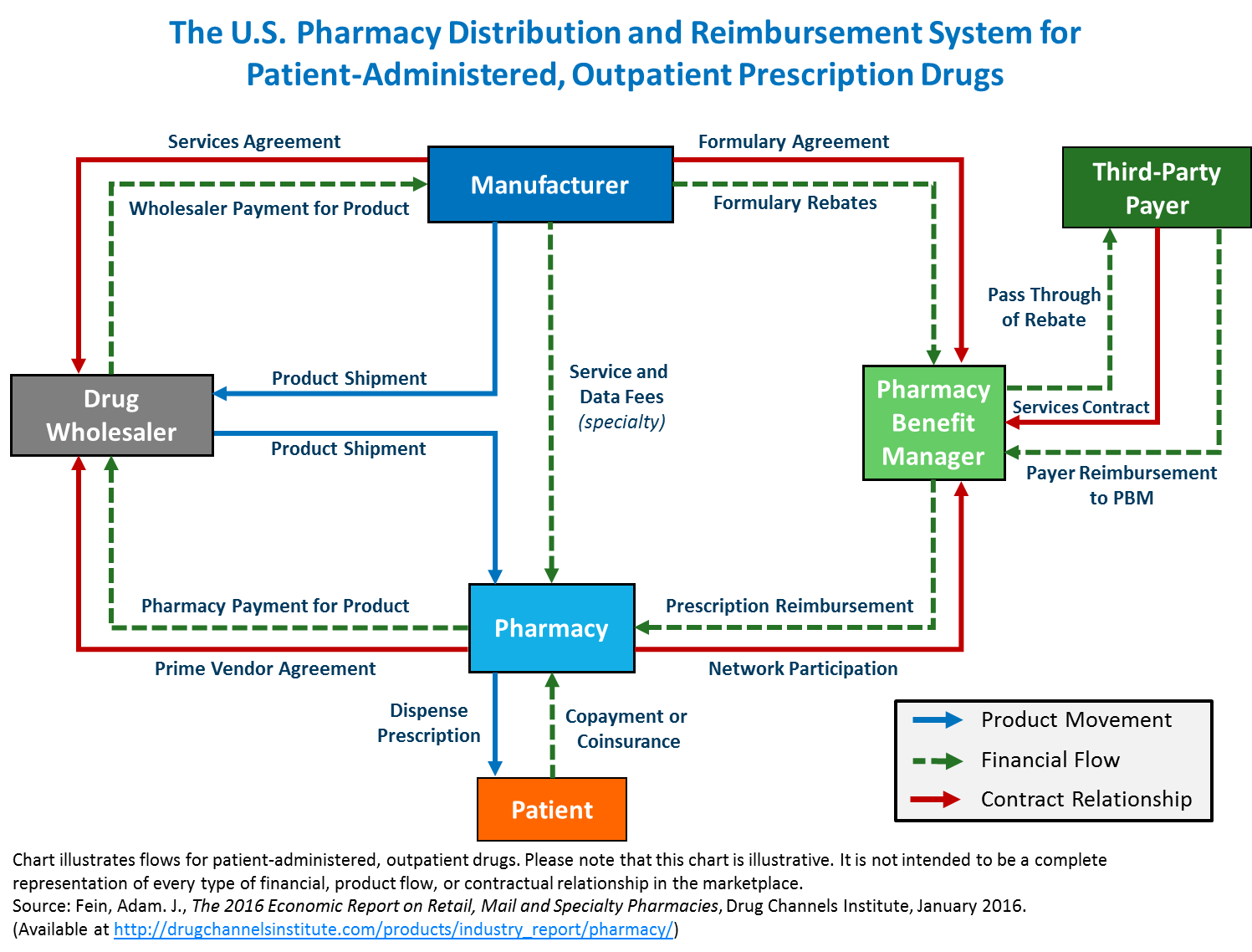
Where PBMs Fit in the Prescription Drug System
Prescription medicines move through a complex system involving manufacturers, insurers, pharmacies, and benefit administrators. Pharmacy Benefit Managers help coordinate many of the processes that connect these parts of the healthcare system.
PBMs negotiate drug prices with manufacturers on behalf of health plans and employers, develop formularies that determine which medications are covered, and administer pharmacy networks that dispense prescriptions to patients.
Because PBMs operate between several key parts of the healthcare system, their policies can influence how medicines are priced, how coverage decisions are made, and how patients ultimately access their prescriptions.